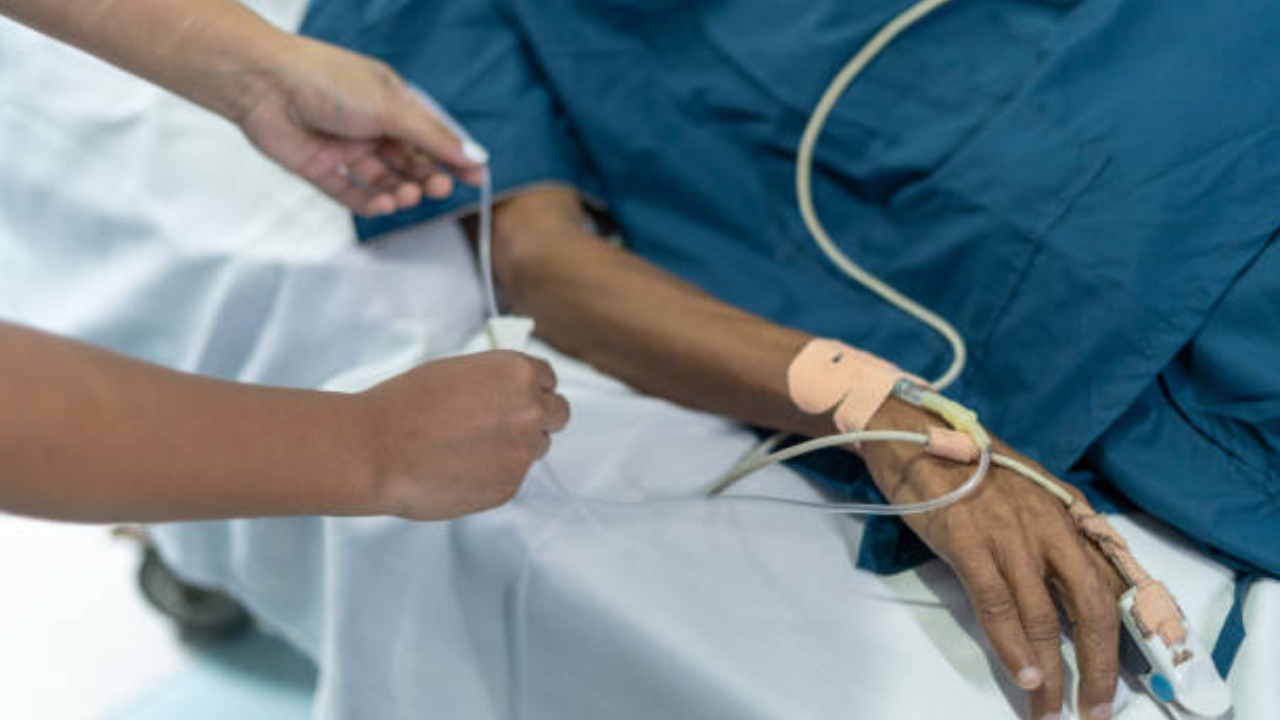
The air in the Equateur Province of the Democratic Republic of Congo does not move. It sits heavy, a thick blanket of humidity that smells of damp earth and woodsmoke. In the village of Bikoro, the silence is not the peaceful quiet of the countryside. It is the strained, brittle silence of a community holding its breath. Somewhere in the dense green periphery of the Congo Basin, a microscopic hunter has slipped its leash again.
Ebola does not arrive with a fanfare. It begins with a headache that feels like heatstroke or the familiar, bone-deep ache of malaria. You ignore it. You go about your day, washing clothes in the river or tending to your crops, unaware that your internal architecture is being systematically dismantled. By the time the fever spikes and the world begins to blur, it is often too late for you—and perhaps for everyone you have touched.
The latest declaration of a large-scale outbreak is not just a headline or a data point on a WHO dashboard. It is a biological firestorm in one of the most logistically challenging environments on Earth.
The Invisible Threshold
Imagine a young father named Jean. This is a hypothetical name, but his story is being mirrored in dozens of clinics across the region right now. Jean carries a heavy bag of charcoal to market, feeling a bit sluggish. He wipes sweat from his brow, leaving a trace of salt and skin cells on his hand. He shakes hands with a neighbor. He hugs his daughter.
[Image of Ebola virus structure]
At this stage, Jean is a walking mystery. The Ebola virus is a filovirus, a long, thread-like strand that looks like a shepherd’s crook under a microscope. It is deceptively simple. It enters the body and targets the very cells meant to protect us: the macrophages and dendritic cells. It hijacks the immune system, using our own defense network as a transit system to reach the liver, the spleen, and the adrenal glands.
The tragedy of Ebola lies in its exploitation of human kindness. In many Congolese communities, caring for the sick is a sacred duty. Washing the bodies of the deceased is a final act of love. But the virus remains most concentrated in the body just after death. The very act of honoring a father or a grandmother becomes the engine of the next cluster of infections. This isn't just a medical crisis; it is a cultural siege.
A War on Two Fronts
The geography of the Congo is a masterpiece of natural beauty and a nightmare for epidemiologists. The Equateur Province is a labyrinth of rivers and swampy forests. There are few paved roads. To reach an affected village, health workers often spend days on motorbikes or in dugout canoes, navigating paths that disappear during the rainy season.
The logistics of a "large outbreak" declaration involve more than just doctors. It requires a massive influx of specialized equipment. Think about the "space suits"—the Personal Protective Equipment (PPE). In the 95-degree heat of the jungle, a health worker can only stay in that plastic suit for about forty minutes before the risk of heat exhaustion becomes life-threatening. They emerge drenched, their boots literally filled with sweat.
Then there is the cold chain.
The modern vaccines we use to fight Ebola, like the rVSV-ZEBOV, are marvels of science, but they are fragile. They must be kept at temperatures as low as $-80°C$. Maintaining that "Ultra-Cold Chain" in a region where electricity is a luxury requires solar-powered freezers, heavy-duty generators, and a constant supply of fuel. Every mile of muddy track is a gamble against the clock. If the freezer fails, the "liquid gold" inside becomes useless water.
The Weight of History
We have to talk about the shadow of the past. This isn't the first time the Red Ghost has haunted the Congo; the virus was first identified here in 1976 near the Ebola River. Since then, the country has faced more outbreaks than any other nation. You might think this makes the response easier, a practiced routine. In some ways, it does. Local scientists and burial teams are among the most experienced in the world.
However, experience breeds a different kind of exhaustion.
The people living in these regions have seen a parade of international NGOs, blue-helmeted UN vehicles, and white Land Cruisers for decades. They have seen billions of dollars flow into "emergency responses" while their daily reality—lack of clean water, crumbling schools, and nonexistent basic healthcare—remains unchanged. This creates a fertile ground for suspicion.
When men in yellow suits arrive to take away a sick relative to a fenced-off "Ebola Treatment Center," the community doesn't always see rescuers. Sometimes, they see strangers stealing their loved ones to die in isolation. Rumors spread like the virus itself: The foreigners brought the disease. The medicine is a poison. The bodies are being harvested. Breaking these myths requires more than a megaphone and a pamphlet. It requires the slow, grueling work of "social mobilization." It means sitting with village elders, listening to their fears, and finding ways to integrate traditional values with modern biosafety. It means proving that the treatment center is a place of hope, not a morgue.
The Mathematics of Mercy
When the government declares an outbreak is "large," they are looking at the effective reproduction number, or $R_0$. In the early stages of an Ebola outbreak, if one sick person infects two others, the growth is exponential.
- One case becomes two.
- Two become four.
- Four become sixteen.
The goal of the response is to push that number below 1.0. This is achieved through a strategy called "Ring Vaccination." Instead of trying to vaccinate millions, teams identify every person who had contact with a confirmed case—the first ring—and then everyone who had contact with them—the second ring. It is a biological scorched-earth policy, creating a human buffer of immunity that the virus cannot leap across.
But the rings are only as good as the data. If a family hides a sick child out of fear, the ring has a hole. If a traveler boards a crowded barge headed toward Mbandaka or Kinshasa, the ring breaks entirely. Mbandaka is a major port city on the Congo River. If the virus hitches a ride on a commercial boat, it has a direct highway to a population of millions. That is the nightmare scenario that keeps health officials awake at night.
The Cost of Looking Away
There is a psychological distance we maintain when reading about an outbreak in a distant forest. We treat it as a "them" problem. But the world is smaller than we care to admit. In 2014, we learned that a single infected traveler can turn a regional crisis into a global panic within forty-eight hours.
The nurses and doctors on the front lines in Equateur are the world's thin red line. They are working with limited resources, often at great personal risk. Some have gone months without seeing their own families. They aren't just fighting for the lives of the people in Bikoro; they are preventing a global catastrophe.
The real tragedy is that we usually only care when the fire is roaring. We fund the "emergency," but we neglect the "preparedness." We buy the fire trucks when the house is burning, but we refuse to pay for the smoke detectors or the fireproof insulation. Strengthening the DRC’s permanent health systems—building clinics that function every day, not just during disasters—is the only way to eventually stop the Red Ghost for good.
The Long Walk Home
Late in the evening, after the heat has finally begun to dissipate, a survivor might be released from a treatment center. This is a moment of profound, complicated joy. In many centers, there is a "wall of survivors" where people leave their handprints in bright paint.
But for someone like Jean, the walk back to the village is daunting. He is "clear," but is he welcome? He carries a certificate of health, a piece of paper that says he is no longer a threat. Yet, his neighbors might still move their chairs away when he sits down. His bedsheets were likely burned by the disinfection teams. His clothes are gone. He is alive, but he is starting from zero.
The success of an Ebola response isn't measured solely by the final case count or the date the outbreak is declared over. It is measured in the resilience of the people left behind. It is found in the courage of a mother who takes in an orphaned niece, knowing the risks but choosing love anyway. It is found in the local lab technician who spends twelve hours a day analyzing blood samples under a flickering light bulb.
The forest remains, dark and vast, holding its secrets. We know the virus is out there, likely circulating in bat populations, waiting for the next spillover event. We cannot wish it away, and we cannot hide from it behind borders or rhetoric. We can only meet it with the same things the Congolese people use every day: endurance, communal strength, and an unwavering refusal to let the darkness have the final word.
The sun sets over the river, turning the water the color of bruised plums. Somewhere in the trees, a bird cries out, and a health worker zips up a suit for the night shift. The battle continues, one heartbeat at a time.